Wolff-Parkinson-White Syndrome
The heart has 4 chambers that pump blood. The 2 upper chambers are the right and left atria, and the 2 lower chambers are the right and left ventricles. The heart also has an electric system that directs the coordinated beating of these 4 chambers.
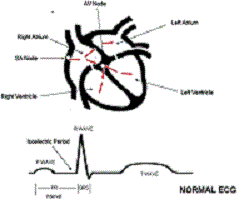
A schematic drawing of the normal heart structure and electric system (red arrows) is shown in Figure 1. A normal electric impulse originates in an area of the upper right atrium called the sinus (SA) node, and an ordinary electric activity of the heart is referred to as normal sinus rhythm. In normal sinus rhythm, an electric impulse is generated by the SA node, and that electricity spreads through the right and left atria, directing these chambers to beat.
On an electrocardiogram (ECG; bottom of Figure 1), the electric activity from the atria is seen as a small rounded deflection called a P wave. The same electric impulse then passes through a small area of tissue between the atria and ventricles called the atrioventricular (AV) node and then down through the ventricles. On the ECG, the electric activity from the ventricles results in a larger deflection called the R wave or QRS complex. Because the AV node is small, there is not enough electric activity to cause a deflection in the ECG. Therefore, the time spent by the electric impulse traveling through the AV node is represented on the ECG by a flat interval called the PR interval. In a normal heart, the AV node is a gatekeeper of sorts in that it is the only pathway for electricity that communicates from the upper chambers (atria) to the lower chambers (ventricles). The combination of electric impulses from the SA node to the atria, then through the AV node, and down to the ventricles results in 1 heartbeat. In summary, the electric activity on the ECG starts with a small deflection that results from atrial electric activity (the P wave), followed by a flat section resulting from electric activity through the AV node (the PR interval), followed by a larger deflection that results from electric activity from the ventricles (the R wave or QRS complex).
What Is an Accessory Pathway or Bypass Tract?
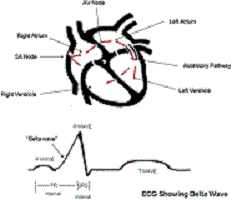
Some people are born with an extra piece of heart muscle tissue that connects directly between the atria and the ventricles, bypassing the AV node altogether. This abnormal piece of muscle is referred to as a bypass tract or an accessory pathway (Figure 2).
This extra piece of tissue can serve as a passageway for the electric signals between the atria and ventricles and allow electric activity in the ventricles to occur immediately after electric activity in the atria without having to wait for the electric impulse to travel through the AV node. In this situation, the ECG may not have much of a flat PR interval but instead may have the P wave (from atrial activity) right up against the R wave (from ventricular activity), with the R wave beginning with an upslope referred to as a delta wave (Figure 2). This delta wave results from electric activity traveling over the accessory pathway and bypassing the AV node.
Some people with an accessory pathway have a normal ECG at baseline because the accessory pathway is electrically active only when there is a fast, racing heartbeat (tachycardia) described below. Therefore, some people with accessory pathways can have completely normal ECGs like the one seen in Figure 1. This is referred to as a concealed accessory pathway.
How Does an Accessory Pathway Cause a Fast Heartbeat (Tachycardia)?
Not all patients with accessory pathways have fast heartbeats. Some people with a delta wave on their ECG caused by an accessory pathway will never have a problem with a fast heartbeat. In others, a rapid heartbeat ( tachycardia) can sometimes suddenly occur. The 3 different types of tachycardias associated with accessory pathways are shown in Figure 3.
The most common type (Figure 3 A) results from an electric circuit that travels from the atria through the AV node to the ventricles, then backward through an accessory pathway to the atria, and then back through the same circuit over and over again. Because this is a circuit that reenters itself and involves the atria and ventricles, it is referred to as AV reentrant tachycardia. The less common type of AV reentrant tachycardia (Figure 3 C) involves a circuit that travels forward from the atria through the accessory pathway and backward through the AV node.
Another type of tachycardia that can be seen in patients with accessory pathways is a chaotic irregular beating of the upper chambers of the heart called atrial fibrillation. If a patient with an accessory pathway develops atrial fibrillation and if that particular accessory pathway is capable of rapid electric conduction, this can lead to an extremely rapid pulse rate, which can be dangerous.
What is Wolff-Parkinson-White Syndrome?
Wolff-Parkinson-White syndrome (WPW) is the combination of accessory pathway activation seen on an ECG (delta waves) and episodes of tachycardia. It was first described in 1930 by Louis Wolff, Sir John Parkinson, and Paul Dudley White. Along with a delta wave, patients have a shorter time between the conduction of an impulse from the atrium to the ventricle, referred to as a short PR interval (see the ECG in Figure 2).
What is described above is called a preexcitation or WPW pattern. The presence of a pattern does not necessarily mean that the patient will experience WPW syndrome. The WPW pattern will be seen in about 0.2% of the general population. Of those patients with the WPW pattern, a minority will experience tachycardia and be defined as having WPW syndrome. WPW can be associated with Ebstein anomaly, a heart defect in which the valve connecting the right atrium and ventricle (tricuspid valve) is abnormally formed and placed lower than normal in the right ventricle. However, in most patients, WPW is not related to any other heart abnormality. It can occur at any age, is often first noted in childhood, but may not be diagnosed until adulthood in some patients. Symptoms of WPW syndrome are usually abrupt and may include palpitations, chest discomfort, and occasionally fainting.
On very rare occasions (less than 0.1% of the time), a patient with WPW can experience sudden cardiac death that results from the development of a chaotic irregular beating in the upper chambers of the heart called atrial fibrillation with rapid conduction down an accessory pathway (Figure 3B) leading to an extremely rapid pulse that can lead to cardiac arrest. Fortunately, this is a rare event in patients with WPW, and there are certain factors that a physician can often identify ahead of time to risk stratify patients with WPW.
Treatment
Treatment of WPW must be individualized. For patients who have only a documented WPW pattern on their ECG but no symptoms and no documented tachycardia, simple conservative observation may be appropriate. When symptoms or documentation of arrhythmias exists, a catheter-based electric evaluation of the heart called an electrophysiology study may be offered. This usually results in elimination of the accessory pathway with cautery delivered through the catheter called radiofrequency ablation. This will also eliminate the WPW pattern on the ECG. On rare occasions, WPW syndrome may be treated with antiarrhythmic medications, although most patients opt for the catheter ablation procedure because it may be curative and eliminate the need for lifelong medication therapy.
Conclusions
WPW syndrome results from tachycardia associated with an accessory pathway. The WPW pattern is diagnosed by a delta wave and/or short PR interval on an ECG. Once symptomatic, patients can be treated with catheter ablation or can try medications to control their symptoms. Management of WPW syndrome should be individualized, and treatment decisions should be carefully discussed with your doctor.
Reference: J.Kulig et al; Circulation 2010; 122: e480-e483.